As the COVID-19 pandemic took hold in early 2020, one of the ways medical professionals were able to continue providing care was through telehealth. Patients were able to connect with their doctors via 2-way video communication technology, either from home via a smartphone app or from an interactive kiosk via a neighborhood clinic.
The U.S. Department of Health and Human Services and the Centers for Disease Control encouraged health care providers to “adopt and use telehealth as a way to safely provide care to your patients in appropriate situations, including: routine health care, like wellness visits; medication consultation; dermatology (skin care); eye exams; nutrition counseling; mental health counseling.” Although the telehealth concept was around before the pandemic, quarantines and social distancing guidelines helped drive 1.6 million telehealth encounters during the period between January and March 2020, double the number of encounters during the same period the previous year.
In addition to making it easy for home-bound patients to receive advice from a professional without having to leave their homes, telehealth allowed those in rural areas to receive care that would otherwise be unavailable. A telehealth kiosk located at a local community center, for example, could allow patients to connect with doctors without having to drive for hours to the nearest city.
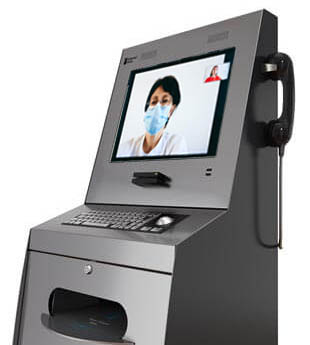 Federal funding to expand the use of telehealth services could be on the horizon.
Federal funding to expand the use of telehealth services could be on the horizon.
Serving the underserved
The CDC continues its support of telehealth, pointing to one study showing that “telestroke” services help increase the use of lifesaving treatments and that telehealth was proving to be successful in delivering programs for issues such as Type 2 diabetes prevention and cardiac rehab.
And states are looking at telehealth kiosks to provide care in areas where hospitals have closed or are too far away for residents to access. Texas, for example, is testing the use of telehealth kiosks to fill the vacuum left by the closure of 26 rural hospitals over the last decade. Thirty-five of the state’s 254 counties currently have no physicians. In Reading, Pa., a telehealth kiosk at a rescue mission provides basic health services to the homeless. In Nebraska, healthcare providers are looking at kiosks as a way to provide services to Native American populations, which have typically been underserved when it comes to health care.
The federal government has taken several steps throughout 2021 to pave the way for telehealth expansion in rural and underserved communities. In August, the Biden administration awarded $19 million to 36 organizations through the Health Resources and Services Administration at HHS to expand such services and foster telehealth innovation and quality. In addition, the recently passed Infrastructure Investment and Jobs Act included $65 billion to improve access to broadband Internet service, a critical part of delivering telehealth services.
There are additional actions under consideration that could further enhance access to telehealth kiosks.
All 50 states and the District of Columbia waived parts of their medical licensing requirements during the pandemic, paving the way for patients to connect with out-of-state doctors. Someone in Virginia seeking mental health care, for example, could connect with a doctor in New Jersey via video chat for treatment. As long as the doctor was licensed in New Jersey they didn’t need to be licensed in Virginia while the waivers are in place. Many health insurers also covered telehealth services during the pandemic.
Although some states have begun rolling back those licensing waivers as the pandemic appears to be on the wane, some health care advocates are seeking to make them permanent. Eliminating the waivers, they say, threatens to cut many patients off from the care they need.
Federal legislation under consideration that is designed to address those issues, and others, include the bipartisan Expanded Telehealth Access Act, which would make telehealth visits for physical therapy services and other rehabilitation services permanently available and billable under Medicare. The Creating Opportunities Now for Necessary and Effective Care Technologies (CONNECT) for Health Act of 2021 would also address many of those issues, and allow health centers and rural health clinics to provide telehealth services. That bill has the support of 50 senators and 150 health care organizations.
Telehealth services likely to expand
The COVID-19 pandemic changed the way health care is delivered, and those changes are likely to be permanent.
According to the CDC, people who live in rural areas are more likely than urban residents to die prematurely from the leading causes of death: heart disease, cancer, unintentional injury, chronic lower respiratory disease, and stroke. Expanding the use of telehealth kiosks is one way to address those issues.
To see how Advanced Kiosks can help with your telehealth kiosk project and for more info on how a telehealth kiosk can benefit your organization, reach out to one of our experts.










